Danger in the jungle

The dangers in the jungle depend on the particular region of the country. Least of all the dangers of the tropical islands of Polynesia, the most in the equatorial islands of Micronesia and Asia. In many countries, should be afraid of crocodiles, snakes, spiders, poisonous frogs. Just everywhere should beware of sharks, barracudas, stingrays, moray eels in the open ocean. WARNING! Before you go to the jungle - take care of that you have received all vaccinations! Hepatitis A, B, polio, measles, tetanus, yellow fever, smallpox, diphtheria, tuberculosis. In some countries you simply can not miss for example no vaccinations against yellow fever.
Yellow fever
The incubation period ranges from 3 to 6 days, sometimes up to 10 days. The disease varies in severity from a mild fever to severe hepatitis with hemorrhagic fever. Heavy flow is characterized by a sudden onset, accompanied by fever up to 39-41 ° C, chills, severe headache, pain in the muscles of the back and extremities, nausea, vomiting. Characterized by the appearance of the patient: icteric staining of the skin due to liver damage (hence the name of the disease), his face red, puffy, swollen eyelids. After a brief period of light may come a shock, hemorrhagic syndrome with the development of acute renal failure, acute liver failure. Flowing at lightning speed development of the disease the patient dies within 3-4 days. The mortality of the disease ranges from 5-10% to 15-20%, and during epidemic outbreaks - up to 50-60%. Yellow fever refers to a quarantine disease.
We have had a disease people have lifelong immunity.
Specific drugs for the treatment of yellow fever. Assistance is reduced to symptomatic treatment include rest, the use of non-steroidal anti-inflammatory drugs, infusion solutions should be avoided acetylsalicylic acid (Aspirin)!
The carrier - mosquitoes.
Yellow fever is found only in South America and Africa! In Asia and Oceania, it is not!
Vaccine is considered to be one of the most secure and highly efficient vaccines in the history of vaccinology. Reliable immunity develops within one week in 95% of vaccinees and stored for 30-35 years (possibly lifetime).
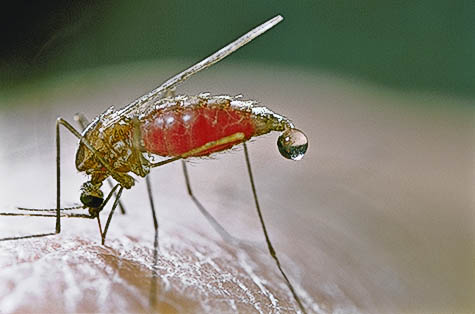
Malaria
Malaria symptoms usually include fever, chills, arthralgia (joint pain), vomiting, anemia caused by hemolysis, hemoglobinuria (separation of hemoglobin in the urine), and convulsions. Perhaps also a tingling sensation in the skin. May also have splenomegaly (enlarged spleen), unbearable headache, cerebral ischemia. Malarial infection is deadly.
The most common medications for the treatment of malaria today, as before, is quinine, chloroquine, doxycycline. Used for the treatment of Coartem (Coartem) - this drug is considered to be the best. Kills all species of malaria parasites. The course of treatment 3 days to 4 tablets in the morning and in the evening (of 24) Just sell special test strips (as in pregnancy) With it you can determine the version of the deadly malaria P. falciparum For the prevention of malaria using a number of medications: chloroquine (0.5 g), galohin (0.3 g), hloridin (0.025 g), and others paludrin Reception of one of the following drugs should be started from the first day in the jungle and spend one times per week.
Schistosomiasis

Tropical parasitic disease caused by blood flukes (trematodes) of the genus Schistosoma. Dermatitis is characterized by a period of the introduction of parasites in the skin and the subsequent development of fever, intoxication, urticaria, splenomegaly, eosinophilia, intestinal lesions, or urinary tract.
The clinical picture in schistosomiasis is caused mainly by the development of immunnoallergicheskoy response to parasite eggs. Intestinal schistosomiasis can cause abdominal pain, diarrhea, and blood in the stool.
The classic sign of urinary schistosomiasis is haematuria (blood in urine). In advanced cases often develop fibrosis of the bladder and ureters and kidneys are affected. In men, urinary schistosomiasis can lead to the development of pathology of the seminal vesicles, prostate, and other organs.
Treatment - Praziquantel
Dengue Fever
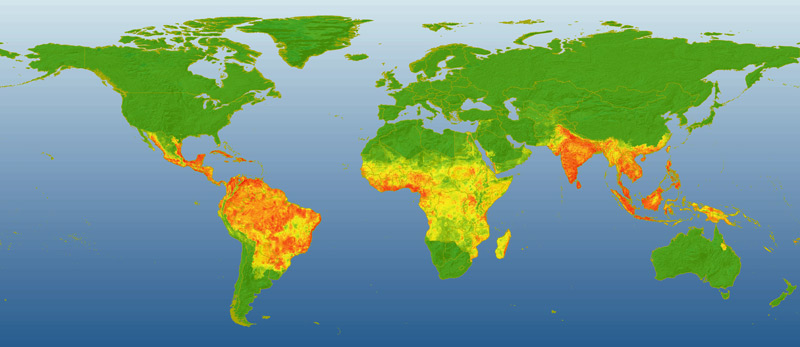
Dengue Fever mapAcute transmissible viral disease. Occurs with fever, intoxication, myalgia, arthralgia, rash and swollen lymph nodes. In some variations, dengue hemorrhagic syndrome develops. Dengue fever occurs mostly in the South and South-East Asia, Africa, Oceania and the Caribbean. Mainly occurs in children and newcomers to endemic areas of the face. The source of infection is a sick man, monkeys and bats. Transmission of infection from an infected person carry out the mosquitoes (Aedes aegypti) and the person (Aedes albopictus) in monkeys.
The incubation period is an average of 3-15 days (usually 5-7 days). The classic dengue fever (sick people with primary infection)
- chills
- bone pain (usually in the spine)
- joint pain (particularly knees)
- muscle pain
- raising the temperature to 39-400C (by the end of the third day the temperature dropped sharply, and after 1-3 days, rises again, then again down 2-3 days)
- anorexia (not eating due to lack of appetite)
- weakness (sharp breakdown)
- nausea
- dizziness
- insomnia
- redness and swelling of the face
- redness of the eyes
- redness of the throat
- increased heart rate at the beginning of the disease, and in 2-3 days it greatly slows
- Different itchy rash (rash appears first on the trunk and then spreads to the limbs and stored 3-7 days)
Dengue hemorrhagic fever (Philippine hemorrhagic fever, Thai hemorrhagic fever, Singapore hemorrhagic fever) - the acute form of classical dengue fever. It develops only from local residents in areas endemic for the disease. Hemorrhagic form occurs with repeated infection with different strains of the virus and is manifested by the following symptoms:
- rise in body temperature to 39-400C
- cough
- anorexia
- nausea
- vomiting
- Abdominal pain
- hyperadenosis
- enlargement of the liver
- marked weakness
- petechial rash (bleeding on the skin)
- gingival, gastrointestinal bleeding
- vomiting blood
- decreased blood pressure, increased heart rate
- pallor, cyanosis of the skin
Patients admitted to a hospital. In the classic form of the disease is prescribed: painkillers, vitamins, antihistamines. In hemorrhagic form of the disease is prescribed: infusion therapy, the introduction of plasma and plasma substitutes (in severe cases), glucocorticoids (in severe cases), oxygen therapy, anticoagulants of direct action.
Typhoid fever
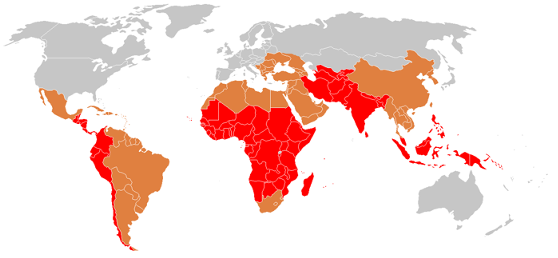
The spread of typhoid fever: red - belt fever, orange - endemic areas of gray - sporadic cases
Pathogen - Salmonella enterica. Typhoid bacteria are quite stable in the environment: in fresh water ponds, they are saved to a month on vegetables and fruit - up to 10 days, and in dairy products can multiply and accumulate. The mechanism of transmission by fecal-oral. The route of transmission - mainly water, but there may be food and household transmission. Transferred disease leaves a strong immunity.
Typhoid fever can be mild, moderate and severe forms. Distinguish atypical form of the disease - abortive and worn.
The course of therapy before the 10th day of normal body temperature regardless of the severity and speed of clinical recovery of the patient. If within 4-5 days no change in the state - to cancel and appoint another. Chloramphenicol (chloramphenicol). adults inside for 20-30 minutes before a meal of 50 mg / kg / day for 4 doses. After normalization of body temperature? 30 mg / kg / day. In case of failure of oral (nausea, vomiting, epigastric pain) parenterally - chloramphenicol succinate 3 grams per day or ampicillin: adults inside after eating at 1-1.5 g 4-6 p / s or parenterally 6 g / s. trimethoprim (80 mg tablets) and sulfamethoxazole (400 mg tablets) - biseptol, bactrim, septrina, cotrimoxazole. adults inside of 2 tablets 2 r / d after a meal (with severe forms of 3 tablets) for 3-4 weeks.
Tetanus

The causative agent of acquired pathogenic properties only in contact with the damaged tissue of a living organism deprived of oxygen. Especially dangerous are chipped or have deep pockets wounds where anaerobic conditions are created.
The disease can develop in deep wounds and injuries of the skin and mucous membranes, burns, frostbite, at birth, the newborn through the umbilical cord, trimmed with non-sterile instrument, as well as certain inflammatory diseases in which inflammation is created hearth contact with the environment (gangrene, abscesses, ulcers, decubitus ulcers, etc.).
A common cause of infection of the lower limbs are microtrauma - wounds, injections with a sharp object, spines, even splinters. Thus, the father of the famous Russian poet Vladimir Mayakovsky became infected with tetanus through the scratch left by the needle. Also, the disease can be caused by bites from venomous animals, spiders, etc. (kind of dangerous spiders Poecilotheria)
Disease may precede the headache, irritability, sweating, tension and muscle twitching in the wound. Immediately before the onset of the disease marked chills, insomnia, yawning, pain in the throat when swallowing, back pain, loss of appetite. However, the incubation period may be asymptomatic.
The initial period lasts up to 2 days. The earliest symptom - the appearance of dull nagging pains in the atrium, where at that time there may be a complete healing of the wound. Almost at the same time or after 1-2 days appears lockjaw - tension and spasmodic contraction of masticatory muscles, making it difficult mouth opening. In severe cases, teeth clenched and can not open his mouth.
Developing tonic contraction of the masticatory muscles (lockjaw) and facial muscle spasms, so that the patient has a sardonic smile armor. risus sardonicus: eyebrows raised, mouth stretched wide, his angles are omitted, the face is a smile and cry at the same time.
The patient is subject to immediate hospitalization in a specialized hospital! No options!
Leishmaniasis
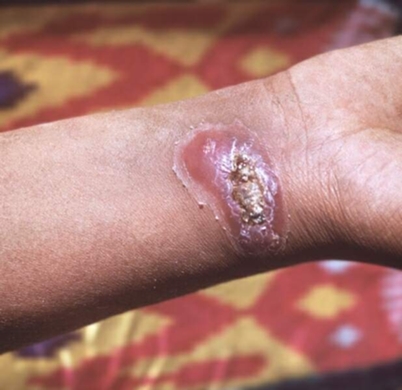
Causative agents of leishmaniasis are protozoa of the genus Leishmania. Distinguish cutaneous, mucocutaneous and visceral forms of infection (visceral).
Depending on the source of infection, leishmaniasis divided into:
- Anthroponotic in which the source of infection is the only person from whom may be infected mosquitoes. Mosquito disease can sometimes be transmitted and other animals, but they are not a source of infection for mosquitoes. These include L. and L. tropica donovani.
- Zoonotic, in which the source of infection are animals - the desert and semi-desert rodents subfamily peschankovyh for L. major, sloths, porcupines and some other South American species of mammals, canines for L. infantum (chagasi).
From human to human leishmaniasis is transmitted.
Used in the treatment of special preparations. If in the course of the disease joins a fungal or bacterial infection, an additional antibiotics or antifungals are appointed.
Rabies

Bat - one of the carriers of rabies in the jungle
The incubation period ranges from 10 days to 3-4 (but usually 1-3) months
Stage 1. Accompanied by a rise in temperature up to 37,2-37,3 ° C, depression, poor sleep, insomnia, anxiety patient. Pain at the bite is felt, even if the wound is healed.
Stage 2. It is expressed in a much higher sensitivity to the slightest stimuli of the senses: bright light, different sounds, noise cause muscle spasms of the limbs. Rabies, hydrophobia. Patients become aggressive, violent, get hallucinations, delirium, a sense of fear.
Stage 3. Paralysis of the eye muscles of the lower extremities. Severe paralytic respiratory disorders cause death. The total duration of illness 5-8 days, sometimes 10-12 days.
In the case of the onset of clinical signs of rabies treatment is not effective! We have to be limited to purely symptomatic agents to facilitate painful condition.
Ciguatera
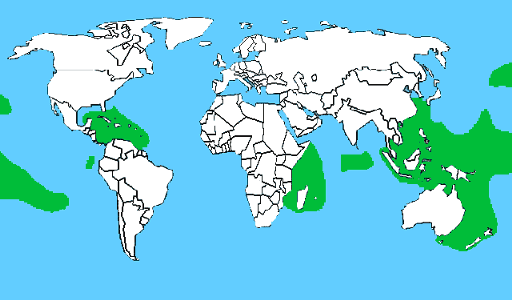
Habitat of fish contaminated with ciguatera
Ciguatera - a disease that occurs when eating certain species of reef fish (pelagic fish, such as tuna, dorado, safe) in tissues that contain a particular biological poison - ciguatoxin.
Ciguatera develops after 1-6 hours after eating the fish. Dominated by symptoms of gastro-intestinal tract, such as abdominal pain, vomiting, diarrhea, but there may be neurological disorders including numbness of tongue and lips, itching, photophobia, metallic taste in the mouth, the replacement of sensations of heat and cold on the opposite . However, in rare cases may occur violations of the respiratory and cardiovascular systems, which can lead to death.
There is no specific treatment. If necessary, the detoxification and rehydration, is symptomatic therapy.
Scolopendra

Scolopendra or millipede reaches a length of 26 cm centipede sacrifice short front legs, plunges into it poisonous maxilliped and begins to chew, sending pieces of food in a wide throat, where they are digested by the enzyme. Eating scolopendra is quite long and slow, making short breaks. Often many times to clean, flowing turns his legs, and then antennae that one or the other side through the maxilliped.
Poison of scolopendra contains acetylcholine, serotonin, lecithin, histamine, thermolysin hyaluronidase. It is well kept in the cold, but is rapidly destroyed by heating under the action of ether: ethyl alcohol, strong alkalis. A person scolopendra bite causes local swelling and pain, usually lasting 1-2 hours if a large scolopendra, these phenomena can be kept for several days, possibly fever, fever, weakness.
Synanceia (Stonefishes)

Stonefish of Synanceia with poisonous spines on the back, which lives at the bottom near the coral reefs and camouflaged under a stone. Is considered the most venomous fish in the world.
The main habitats - coral reefs, near the dark seaweed and stones can also be found resting in the mud or sand. Stonefish - very slow-moving fish. Kept in small areas near the coast, including coral reefs and lava piles. Usually lies huddled in a crevice between rocks or buried in mud or sand. Sticking out of the ground, only the upper part of the head and back, and to them the same stick blade of grass that surround the fish. Notice it is almost impossible, even on land, where it hits the big tides.
On its dorsal part built a number of spikes that produce a poisonous toxin. This is the most dangerous of known venomous fish and its venom causes severe pain with possible shock, paralysis and tissue death depending on the depth of penetration. At the slightest irritation Stonefish raises the dorsal fin spines, sharp and durable, they are easily pierced with men's shoes, accidentally stepped on a fish, and penetrate deep in the leg. With deep penetration of injection can be fatal to humans if it is not received medical attention for several hours.
Sea snakes

Two-tone bonito
Sea snake venom is dangerous to humans. Their venom enzyme prevails that paralyzes the nervous system. When attacking a snake quickly hit two short teeth, slightly curved back. The bite is almost painless, no edema or hemorrhage. But after a while there is a weakness, disturbed coordination, convulsions. From paralysis of the lungs through 7:00 die.
Sea snakes are rarely attack humans, if left alone, they are not happy at all times to avoid the conflict who do not need.
Whiptail stingray

Harmful long, 10-50-inch, serrated tongue and glands that produce venom neurotropic. Prick stingray reminds blow with a blunt knife. The pain rapidly increasing, a 5-1 0 minutes becomes quite unbearable. Local effects (swelling, redness) are accompanied by fainting, dizziness, disturbance of the heart. In mild cases, recovery is rapid, severe - can lead to death from heart failure.
Sea urchins

Dangerous only if they are coming.



